Is it possible that an osteoporosis treatment may destroy my mouth if I get a tooth removed?
- On December 7, 2020
The truth about antiresorptive drugs…
In the middle of the coronavirus pandemic, L came to my dental clinic as she was experiencing toothache. As it was said by her dentist, she was advised to get her premolar removed, but he was hesitant to do it since L was taking a drug that belongs to the group of the so-called bisphosphonates.
L suffers from osteoporosis, also associated with severe arthritis, which makes her feel a lot of pain and involves some mobility problems as well. She came to me quite scared about her dentist’s diagnosis, who refused to remove the tooth because of her medication: bisphosphonates are drugs that can cause medication-related osteonecrosis of the jaw (MRONJ).
Jaw osteonecrosis is a very serious – but rare – pathology: when the cellular renewal process of the maxilla is altered, the cells of the jaw bone start to die due to the action of bisphosphonates or monoclonal antibodies. This can happen after tooth extraction or oral surgery.
There is scientific evidence that more than 190 million bisphosphonates are prescribed all around the globe. Due to the consequences of this treatment, it poses a great challenges to dental professionals and it is increasingly common for them to attend a patient taking antiresorptive drugs in their clinic.
What are bisphosphonates used for?
In general terms, bisphosphonates are used to reduce pain associated with bone problems, to reduce spontaneous fractures in people with osteoporosis, and in cases of cancer, to reduce and control bone metastasis.
But is it true that I cannot have a tooth removed or oral surgery if I take bisphosphonates?
As medical experts, we have to consider a series of factors to answer this question. For this reason, it is advisable to ask your dentist, so s/he can prepare an individual treatment plan completely, adapted to your case. There is a classification of the risk of suffering from osteonecrosis according to the dose that the patient is taking. For example, if it is taken a small dose of bisphosphonates, the risk of suffering from osteonecrosis is extremely low – and 90% of patients take small doses of bisphosphonate.
In 2018, the European Association of Osseointegration (EAO) prepared a consensus document, based on systematic reviews of literature, which was published in “Clinical Oral Implants Research Vol. 29”. From this document were drawn the following conclusions:
- Patients receiving low-dose ARDs (bisphosphonates and denosumab) are at risk of MRONJ, although the risk factor is considered low.
- The risk for MRONJ increases with the duration of drug intake. The effectiveness of drug holidays to mitigate this risk is unclear.
- ARDs are not associated with higher instances of early or late implant failure.
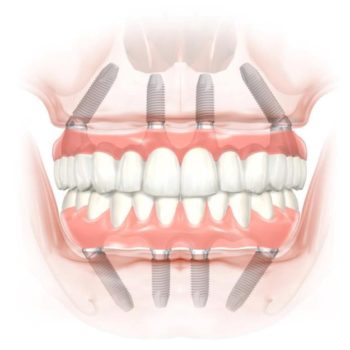
- Low-dose ARDs are not considered a contraindication for implant placement. There is no data available on bone grafting.
- Implant therapy and/or bone grafting procedures are currently not recommended in patients on high-dose ARD intake.
Although zero risk does not exist in any oral procedure, scientific evidence show that we can provide an adequate treatment to those patients who take antiresorptive drugs.
In my opinion, L was not subjected to tooth extraction because her tooth could be restored and not because of taking bisphosphonates. At this time, her oral problem has been resolved and above all, she has more information about oral treatments and their relationship with antiresorptive drugs.
The effect of antiresorptive drugs on implant therapy: Systematic review and meta‐analysis: Andreas Stavropoulos; Kristina Bertl; Peter Pietschmann; Nikolaos Pandis; Morten Schiødt; Björn Klinge. https://www.eao.org/mpage/kpfcp-dd-anti-resorptive-drugs